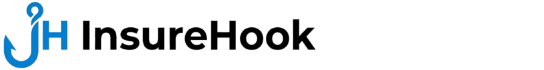Your doctor’s office and your insurance company agree that they will accept your health insurance. You go in. After two weeks, there’s a bill for $340. After 2 weeks, a bill comes in for $340. You had been expecting to pay for your copay $35. What went wrong?
Thousands of times a day, this is the scenario that unfolds in the United States. It’s almost always the same, the cause. The provider was not in-network with the provider/carrier.
One of the easiest tips a health insurance consumer can do is to understand the difference between in-network and out-of-network health insurance. It has a direct impact on the amount of money you pay. Not eventually. Each and every time you utilize your insurance.
In-Network, what does it mean?
Your insurance company doesn’t automatically cover the amount that your doctor bills. It pre-negotiates rates with a select group of providers. A doctor, hospital, laboratory or imaging center that agrees to the negotiated rate is added to your plan’s provider network.
If you utilize one of those providers, you’re going “in-network.” The insurer pays its obligation. Your share is deducted from your deductible, copay, or coinsurance. No numbers are ever going to be random, because they will have been agreed upon by both sides before you get to the door.
Typically, a negotiated rate will be much less than the provider’s billed rate. This discount is only available thanks to the contract between you and your insurer, and the provider. If not, you’ll be charged the provider’s normal charges.
Why Provider Networks Exist
Networks are constructed to manage costs by the insurance companies. Providers become part of a network to have a regular flow of patients. It’s an “appointed” connection that is legally arranged.
Providers who aren’t in networks aren’t necessarily bad. The best specialists in any metro area may well not be a part of all insurance plans. Network exclusion is NOT a measure of quality; it is a business decision.
How Much Does Out-of-Network Care Cost You?
Out-of-network providers are those that do not have a contract with the insurance company. The outcomes will be extremely different depending on your type of health insurance plan. However, the general rule is that you’ll pay more — in some instances, much more.
Some plans will pay some out-of-network benefits. Others don’t provide any at all. When there is partial coverage, the math still may not be in your favor.
Now this is what people don’t expect. Your insurance provider will likely settle out-of-network claims at the amount that it thinks is a “reasonable and customary” charge in your location. That’s an internal benchmark, which is typically lower than the provider’s actual rates. The space in between bills is your responsibility. This is referred to as balance billing.
Patients frequently assume their out-of-pocket maximum protects them from catastrophic bills regardless of network status. In reality, many plans maintain separate out-of-network accumulators. Costs incurred outside the network may not count toward your in-network cap at all.
That is not a technical detail. It is the difference between a $3,000 cap and a $12,000 bill.
Real Cost Comparison: In-Network vs Out-of-Network
The table below reflects typical cost ranges based on common U.S. plan structures. Actual amounts vary by plan, state, and provider.
| Service Type | In-Network Patient Cost | Out-of-Network Patient Cost |
|---|---|---|
| Primary care visit | $20 to $40 copay | $120 to $250 or full billed rate |
| Specialist visit | $40 to $75 copay | $250 to $500+ |
| Urgent care visit | $50 to $100 copay | $200 to $600+ |
| Emergency room | $150 to $350 copay | Covered at in-network rate (No Surprises Act) |
| Outpatient surgery | 10% to 20% after deductible | 40% to 50% or not covered |
| Lab work | $10 to $30 | Full billed rate |
| Mental health session | $20 to $50 copay | $150 to $300+ |
| Imaging (MRI, CT) | 20% after deductible | 40% to 60% or not covered |
Insurance laws and coverage rules vary by state. A plan sold in California may structure out-of-network benefits very differently from one sold in Georgia.
How Your Plan Type Changes Everything
This is where most explanations stop short. The in-network versus out-of-network distinction doesn’t work the same way across all plans. Your plan type determines how strictly the network rules apply.
HMO Plans
HMO plans (Health Maintenance Organizations) operate within strict network boundaries. You choose a primary care physician. That physician coordinates your care and issues referrals to in-network specialists.
Go outside the network for non-emergency care and you typically receive zero coverage. The plan simply doesn’t pay. You absorb the entire cost.
HMOs usually carry lower premiums precisely because the network restriction is so firm. They work well for people with consistent care needs and access to a solid local network.
PPO Plans
PPO plans (Preferred Provider Organizations) give you the most flexibility. You can see any licensed provider. No referral required. Your insurer pays a higher share when you stay in-network and a lower share when you go out.
The trade-off is cost. PPO premiums run higher than HMO premiums. Out-of-network coverage exists but comes with steeper cost-sharing. If you have a complex medical history or see specialists regularly, comparing HMO and PPO structures before enrollment can save you real money.
EPO Plans
EPO plans (Exclusive Provider Organizations) combine features from both. You don’t need a referral to see a specialist. But you must stay in-network for all non-emergency care. Step outside the network and coverage disappears. No partial payment. No exception.
HDHP Plans
High-deductible health plans come in both HMO and PPO formats. The network rules follow whatever structure the plan uses. What makes HDHPs distinct is the large deductible you must meet before coverage activates. Out-of-network care on an HDHP can generate enormous costs before any coverage kicks in.
A Real Scenario Worth Walking Through
Marcus lives in Charlotte and has a PPO plan through his employer. He’s been seeing an orthopedic surgeon for a knee issue and scheduled a procedure for March. His surgeon is in-network. The surgery center his surgeon uses is also in-network.
What Marcus didn’t verify was the anesthesiologist. That provider worked independently. Not contracted with Marcus’s insurer. The surgery went perfectly. The anesthesiology bill arrived six weeks later for $2,100. His insurer paid $400 based on its “usual and customary” benchmark. Marcus owed $1,700.
This scenario isn’t unusual. The No Surprises Act now limits this practice in many situations. But understanding the limits of that law matters.
The No Surprises Act: What It Actually Covers
The No Surprises Act took effect January 1, 2022. It created federal protections against certain forms of surprise medical billing. Understanding what it covers and what it doesn’t is important.
What It Protects Against
The law prohibits balance billing from out-of-network providers in these specific situations:
Emergency services at any facility regardless of network status. Your insurer must cover the visit at the in-network rate. The provider cannot bill you for the difference beyond standard in-network cost-sharing.
Non-emergency services at in-network facilities when you had no practical choice of provider. This includes situations like Marcus’s anesthesiology bill. If an out-of-network provider treats you at an in-network facility without your informed consent, balance billing is prohibited.
Air ambulance services from out-of-network providers are now also covered under these protections.
What It Does Not Cover
Ground ambulance services remain outside the law’s protections in many cases. Out-of-network care you intentionally and knowingly choose is not protected. If you sign a consent form agreeing to out-of-network care and waiving protections, you can still be balance billed.
The Centers for Medicare and Medicaid Services provides detailed guidance on these protections at cms.gov/nosurprises.
Verifying Network Status: The Right Way
Most people check the insurer’s online provider directory. That’s a reasonable starting point. It’s not enough on its own.
Provider directories have a known accuracy problem. The federal government has flagged this repeatedly. Providers join and leave networks throughout the year. Directories don’t always update in real time. A provider listed as in-network today may have terminated their contract last month.
Steps That Actually Work
Call your insurance company directly. Ask them to confirm in-network status for the specific provider using their NPI number (National Provider Identifier). Write down the date, the representative’s name, and the confirmation number if one is given.
Call the provider’s billing office. Give them your plan name, plan ID, and group number. Ask them to confirm participation. Not just “we accept your insurance.” Confirm they are contracted with your specific plan.
For any scheduled procedure at a hospital or surgery center, ask your care team to identify every provider who will be involved. Surgeons, assistants, anesthesiologists, radiologists. Confirm each one separately.
Many plans also allow you to request an exception if no in-network provider is available for a needed service. This process is called a network adequacy exception or gap exception. Your insurer’s cost-sharing structure will specify how these are handled.

Out-of-Pocket Maximums and the Network Trap
Your out-of-pocket maximum is the most a plan will make you pay in a plan year for covered services. After you hit that cap, the insurer pays 100% for the rest of the year.
Here’s the catch most people miss.
Many plans set separate out-of-pocket maximums for in-network and out-of-network care. Spending $6,000 on out-of-network care may not count toward your in-network cap at all. You could hit your in-network maximum and still face unlimited out-of-network costs if you continue seeing non-contracted providers.
Federal rules under the Affordable Care Act set a maximum cap for in-network costs. For 2026 that cap is $9,200 for individuals and $18,400 for families on most marketplace plans. No equivalent federal cap exists for out-of-network spending on plans that offer partial out-of-network coverage.
Read your plan’s Summary of Benefits and Coverage document. It must disclose whether in-network and out-of-network costs share the same accumulator or track separately. This single detail can have enormous financial consequences.
When Going Out-of-Network Is the Right Call
Not every out-of-network situation is a mistake.
If you have a rare diagnosis and the leading specialist in the country doesn’t participate in your plan, the care quality argument can outweigh the cost argument. Some conditions have very few truly experienced providers. Geographic distance, subspecialty expertise, and clinical outcomes sometimes justify the premium.
If you’re a freelancer or sole proprietor building your own coverage, the network question becomes even more strategic. Health insurance options for self-employed individuals often involve navigating narrower networks to keep premiums manageable. Knowing in advance what you’re trading off matters.
Short-term coverage and gap plans approach the network question very differently. Those products often have narrow or non-existent networks. Understanding that before purchase is critical.
Telehealth and Network Status
Telehealth visits are subject to the same in-network rules as in-person care. A virtual appointment with an out-of-network provider still generates out-of-network cost-sharing.
Some insurers contract with telehealth platforms directly. Others expect you to verify each virtual provider through the standard directory process. With telehealth use expanding across all age groups, this is worth confirming before your first virtual visit. Telehealth insurance coverage varies widely by plan and has seen significant regulatory changes since 2020.
Preventive Care and Network Rules
Preventive care deserves a separate mention. Under the Affordable Care Act, most plans must cover a defined set of preventive services at zero cost-sharing when received in-network. Annual physicals, certain screenings, vaccinations. If you receive those same services from an out-of-network provider, the zero-cost-sharing protection disappears. You pay.
This is one of the clearest examples of where network status produces a direct and immediate financial difference. How preventive care works within your health plan explains which services qualify and how to access them without triggering cost-sharing.
What Changes at Open Enrollment
Networks change every year. A provider in your network this plan year may not be in your network next year. Insurers renegotiate contracts annually. Providers drop plans. New ones are added.
Before you auto-renew your current plan during open enrollment, verify that your most important providers remain in-network. Check your primary care physician, any specialists you see regularly, your preferred hospital, and your pharmacy if it’s a specific concern.
Switching plans to save on premiums can quietly eliminate access to providers you’ve been seeing for years. The relationship between premium costs and network access is one of the most important trade-offs to understand before you finalize enrollment.
The National Association of Insurance Commissioners offers state-specific resources on insurance rights and complaint processes at naic.org.
Network Status Cost Estimator
See your estimated cost difference between in-network and out-of-network care.
These are educational estimates only. Actual costs depend on your specific plan, provider, state regulations, and whether your deductible has been met. Always verify with your insurer before receiving care. Coverage rules vary by state.

FAQs
Yes. Your physician can refer you to any provider they choose. Confirming network status for any referral is your responsibility. Always ask the referring office to help you identify in-network alternatives if the referred provider is out-of-network.
No. It covers specific situations: emergency care, certain non-emergency care at in-network facilities without your consent, and air ambulance services. Intentional out-of-network care you agree to is not protected. Ground ambulance services remain largely unprotected at the federal level.
It depends entirely on your plan. Some plans use a combined accumulator. Many maintain separate in-network and out-of-network limits. Read your Summary of Benefits and Coverage document. Look for the section on out-of-pocket limits and how costs accumulate.
It’s a formal request to your insurer asking them to cover out-of-network care at in-network rates because no in-network provider is reasonably available for your specific condition or location. Approval is not guaranteed. Document your request and follow your plan’s appeal process if denied.
Almost always yes. Most plans build networks around geographic regions. Relocating typically means your current providers are no longer in-network. Moving usually qualifies you for a special enrollment period to choose a plan with an appropriate network in your new location.
Yes. Any time you change plans your deductible and out-of-pocket accumulator reset to zero under the new plan. This is one reason mid-year plan changes can create unexpected cost exposure.
This article is intended for general informational purposes only. It does not constitute legal, medical, or financial advice. Health insurance coverage rules, network requirements, balance billing protections, and cost-sharing structures vary by plan type, insurer, and state. Federal rules referenced reflect regulations in effect as of 2026. Always review your specific plan documents and consult a licensed insurance professional for guidance tailored to your situation.